DIOS-SG
Duodeno-Ileal Omega Switch with Sleeve Gastrectomy
General information
General information
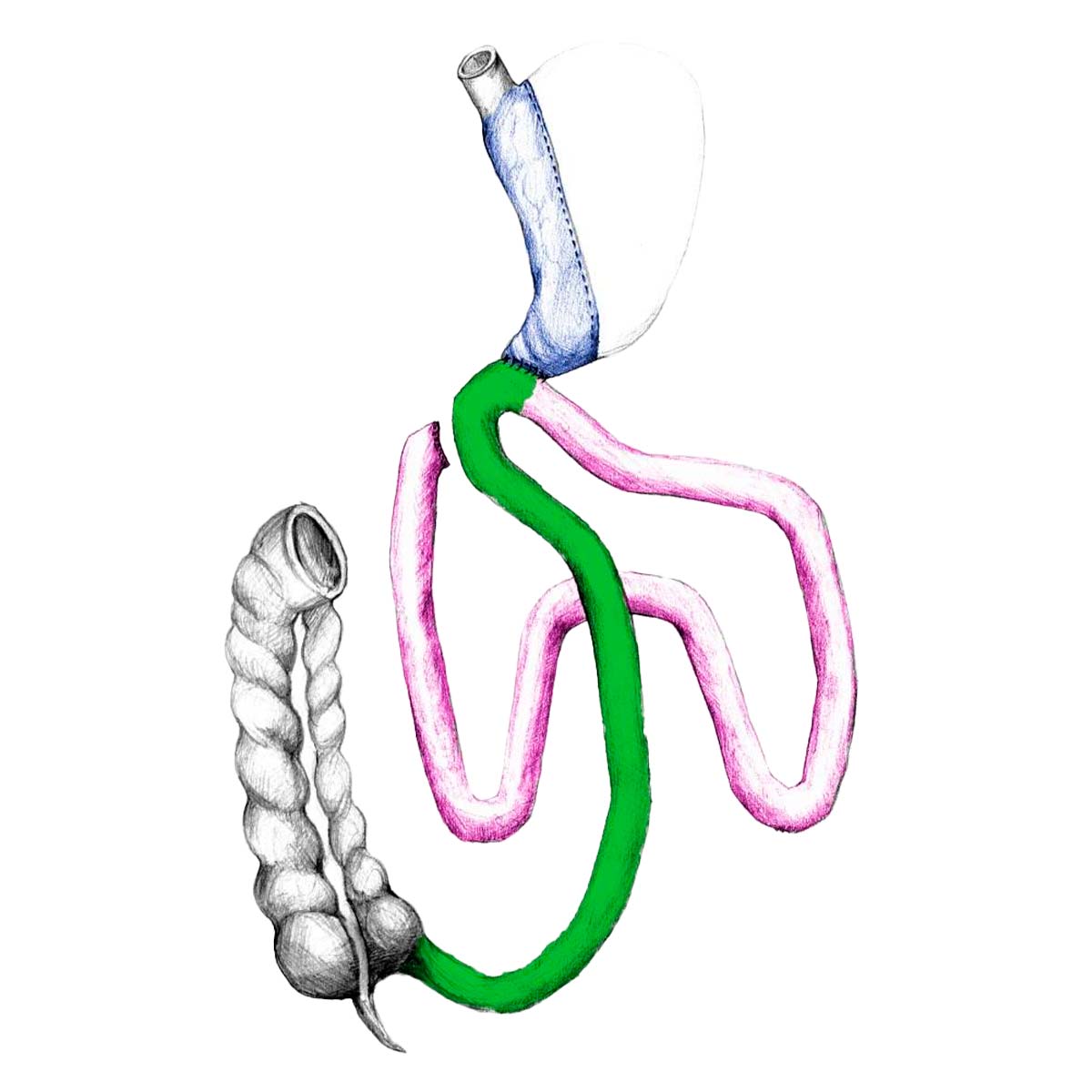
Duodeno-Ileal Omega Switch with Sleeve Gastrectomy is a surgical procedure that can be performed using miniinvasive surgical technology. The procedure influences food intake (restriction-sleeve gastrectomy) and strongly reduces the absorption of nutrients from the intestinal tract. Absorption of nourishing ingredients is limited because a large part of the intestines is bypassed and not used. The food is processed so quickly that there is less time for digestion. The volume of the stomach after DIOS-SG is between 150 and 200 ml, the active intestinal tract – common channel (where the food and digestive fluids come together) is between 200 and 300 cm long.
Facts
Duration of surgery
between 90 and 120 min
Anaesthesia
general anaesthesia
Hospitalisation
4-7 days
Typical patient
- patients with BMI over 45
- patients who accept obligatory supplementation of vitamins and minerals
- sweet eaters
- binge (volume) eaters
- stress eaters
- patients with heartburn
Before Surgery
Indications for DIOS-SG
- BMI over 45
- treatment of:
– diabetes mellitus type 2
– arterial hypertension
– hyperlipoproteinemia
– other related diseases - redo surgery after other metabolic operations in patients with high compliance
- accepts obligatory supplementation of vitamins and minerals
- sweet eaters
- binge (volume) eaters
- stress eaters
Advantages
- very successful (70-90% of excess weight loss)
- operation for patients, where restrictive procedures like Balloon Banding and Sleeve Gastrectomies have failed
- operation for volume eaters
- operation for stress eaters
Disadvantages
- irreversible change in the anatomy
- lifetime vitamin and mineral supplementation after surgery
- foul smelling flatus
- flatulence
- diarrhoea
- sometimes malabsorption
The Surgery
Indication for 2-step procedures
- BMI over 60 or
- BMI over 50 with high perioperative risks
What is a 2-stage operation?
Certain patients may have a body shape that makes their surgery more technically difficult. For example, patients with a BMI over 60 — particularly those who carry their weight in their belly area — may be at increased risk for bariatric surgery. If you fall into this category, you may benefit from 2-stage bariatric surgery. In the staged approach, a multi-step operation like the Gastric Bypass or the Duodenal Switch is broken down into 2 simpler and safer operations. In the first stage, a Sleeve Gastrectomy is performed. This allows you to lose 80 to 100 pounds (ca. 40-50 kilos/ca. 6.5-8 stones) or more, which will make the second part of the operation substantially safer. The second stage operation is usually performed 8 to 12 months after the first. The “sleeve” stomach is converted into a formal gastric bypass. This will permit additional weight loss. Both stages of the surgery can be performed as keyhole surgery, with the advantages of shorter recovery, shorter incisions, fewer incision related problems and less pain.
Technical description
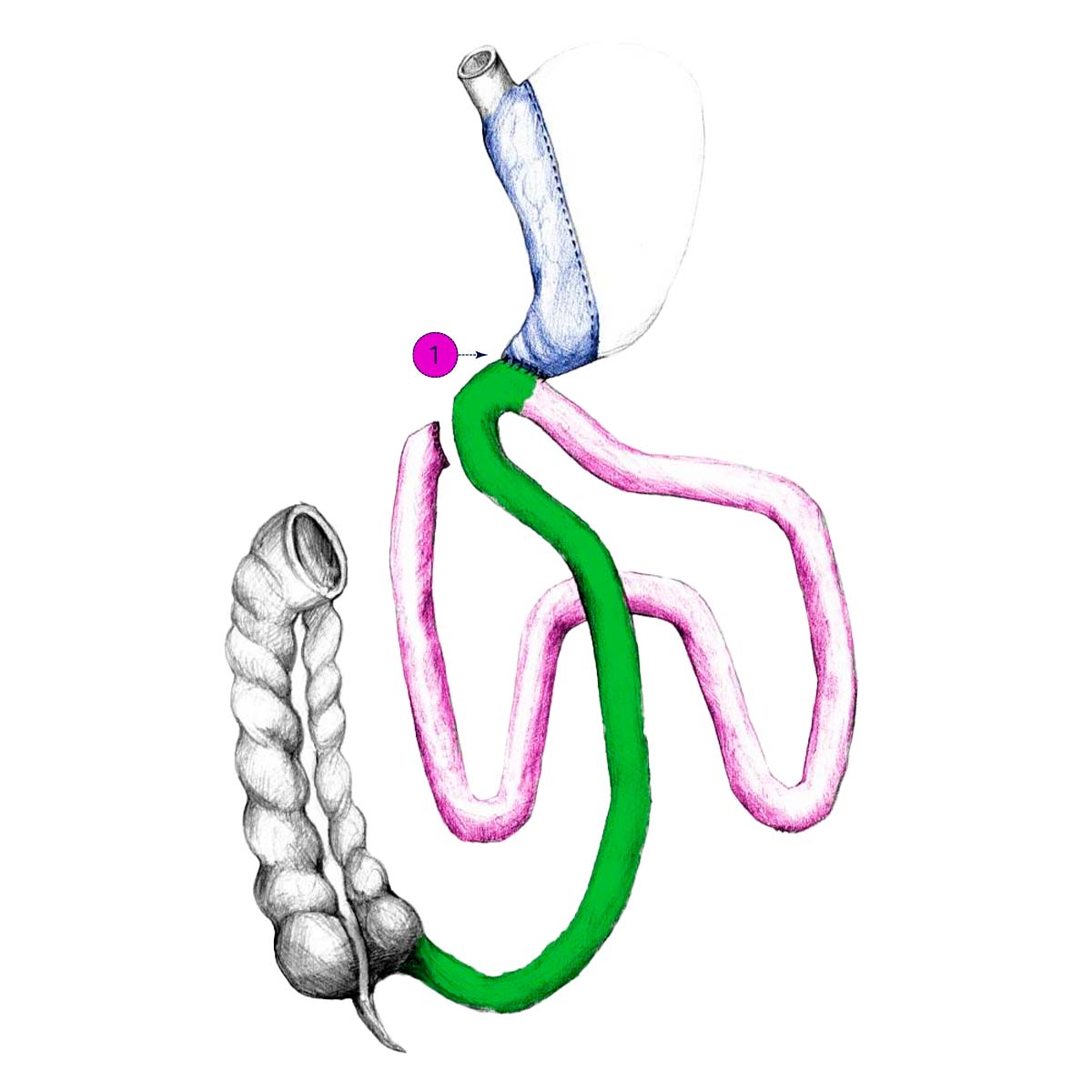
Laparoscopic DIOS-SG reduces the size of the stomach through surgical vertical stapling (Sleeve Gastrectomy). This type of weight loss surgery cuts the stomach and leaves a reservoir of approximately 150 – 200ml in size. Then, distances are measured: the 1/3 of the distal small intestine. Then the intestinal junction is created (called Duodeno-Ileo Anastomosis DIA) with GIA or hand suture between the Duodenum and Jejunum. The connection directs the food immediately from the stomach to the last 1/3 part of the intestines. The first 2/3 of the intestines is now bypassed and is not used anymore for food absorption.
After Hospitalisation
Lab tests
- Morphology
- Electrolytes
- Ferrum
- Creatinin
- Liver ferments
- Vitamins B1, B12-level
- HDL, LDL, VLDL, Chol
- Ferritin
- Transferrin
- Zinc
- Magnesium
- 1,25-Dihydroxy-Vitamin D3, Vitamin A
- Haemoglobin A1c
- Parathormon
- Parathormon – Related Protein
* after three and six months, then annually
Supplementation
- Calcium with Vitamin D3 2000 mg (with 130ug) per day
- Multivitamin + Minerals 1 tab. per day
- Fe+2 Iron 1 tab per day 30mg – one week long in a month, (3 weeks without the Ferrum)
- Protein 70-90g per day
- Vitamin B12 every 3 months i.m. (1000ug) or 25000 I.U. sublingual 2 times a week
- Vitamin A 1 tab. 1mg per day
- Vitamin B1 1 tab. 2.5mg per day
- Zinc 1 tab.15 mg per day
- Biotin, Selenium, Vitamin B9 (B11) daily for 4 months
Standard Medication after Operation
PPI 20 mg, 0-0-1 (3 months)
Sport and physical activity
- 3 weeks after operation – rest
- more than 3 hours of physical activity per week – sport
medical supervision and medical advice required
Weight loss differences
The EWL after BPD-DS reached 80 – 90 % after three years in the best series.
After the second or third postoperative year, the patient seems to adapt to the surgery and to suffer its side-effects in lower intensity, which brings a tendency to regain some of the lost weight.
Important tips
A team of experts must approve the surgery before DIOS-SG operation.
Because we promote safe practice and your safety is of paramount high importance to us and to you, the disadvantages and advantages of the different procedures will be carefully explained to you in detail on consultation.
In the preoperative period, you are provided with care from physicians, psychologists and nutritionists. This team of experts will give you accurate advice on all aspects of the postoperative period: What you can eat and drink, when and how often; what kind of exercises to perform; which individual therapy is necessary for specific issues related to your obesity.
You will have every opportunity to reduce your weight and improve your health. Just imagine the moment when you can wear size L clothes again. Discover your potential and improve your lifestyle. After surgery, you will normally lose approximately 50 kg in first 6 months, provided that you follow the nutrition plan, take exercise therapy and participate in scheduled group discussions.
Only if you are willing to change yourself you will achieve your goal, i.e. healthy weight loss. You must be aware that this will not always be easy. However, with every pound lost, you will win more quality of life, health and a longer life expectancy.
